NEW DIRECTIONS
"No one, except the researchers, had any idea what was going on. They just thought they were getting medical care."
- Carol Kaesuk Yoon, investigative reporter, in a student e-mail interview (2014)
THE STUDY MOVES ON
“They were subjects, not patients; clinical [research] material, not sick people.”
- John Heller, assistant of Dr. Vonderlehr, director of the USPHS Division of Venereal Diseases (1933)
During the summer of 1933, Clark retired from his position as director of the USPHS Venereal Disease Division. Under the guidance of the new chief, Vonderlehr, the study was extended. As new ideas were incorporated, doctors disregarded the rights of study subjects and moral responsibility they should have upheld.
"At the end of this project we shall have a considerable number of cases presenting various complications of syphilis, who have received only mercury and may still be considered untreated in the modern sense of therapy. Should these cases be followed over a period from five to ten years many interesting facts can be learned regarding the course and complications of untreated syphilis."
- Dr. Vonderlehr, director of the USPHS Division of Venereal Diseases to Dr. Clark, preceding director (1933)
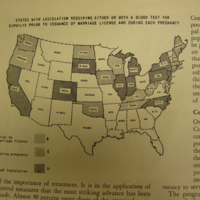
Taken from "an article by R.A. Vonderlehr in Survey Graphic giving an update on the state of syphilis control in the US"
(Venereal Disease Visual History Archive 1940).
(Venereal Disease Visual History Archive 1940).
AUTOPSIES
"As I see it, we have no further interest in these patients until they die."
- Dr. Wenger, director of the PHS Venereal Disease Clinic in Hot Springs, Arkansas in a letter
to Dr. Vonderlehr, director of the USPHS Division of Venereal Diseases (1933)
to Dr. Vonderlehr, director of the USPHS Division of Venereal Diseases (1933)
|
To provide "pathological confirmation" for the study findings, Vonderlehr decided “the proper procedure [was] the continuance of the observation of the Negro men used in the study with the idea of eventually bringing them to autopsy” (Lederer n.d.).
Except from the documentary "Deadly Deception"
|
LETTERS BETWEEN WENGER AND VONDELEHR
|
"If the colored population become aware that accepting free hospital care means a post-mortem, every darkey will leave Macon County and it will hurt Dibble’s hospital.”
- Dr. Wenger, director of the PHS Venereal Disease Clinic in Hot Springs, Arkansas in a letter to Dr. Vonderlehr, director of the USPHS Division of Venereal Diseases (1933)
|
|
“It is not my intention to let it be generally known that the main object of the
present activities is bringing men to necropsy." - Dr. Vonderlehr, director of the USPHS Division of Venereal Diseases, in a letter to Dr. Wenger, director of the PHS Venereal Disease Clinic in Hot Springs, Arkansas (1933)
|
|
"This matter of autopsies is of tremendous importance. There are, as you know, only two other studies that even remotely resemble this--the one started by Bruusgaard in Norway and the study of Rosahn at Yale. So far, of the 173 deaths recorded for the Alabama group 67 percent have come to autopsy. The correlation of postmortem findings with periodic clinical findings can be done only in the Alabama group."
- Dr. Wenger, director of the PHS Venereal Disease Clinic in Hot Springs, Arkansas in a letter to Dr. Vonderlehr, director of the USPHS Division of Venereal Diseases (1933)
|
|
The study soon proceeded to attain the rights to perform autopsies on deceased patients. In a later report from 1953, Nurse Rivers wrote that “to maintain [the subjects’] interest … free medicines, burial assistance or insurance, free hot meals on the days of examination, transportation to and from the hospital, and an opportunity to stop in town on the return trip … all helped” (Public Health 1953).
"It was a picnic atmosphere. We did the bloods, then we'd eat sandwiches, and they'd all sit around and sing. We had fun." - Dr. Olansky, Director of the Tuskegee
Study from 1950 to 1957 |
|
Postmortem examination required the permission of family members of the study participants. As an incentive, the USPHS granted a $50 burial stipend to those who consented to their deceased family member's autopsy.
"The Milbank Memorial Fund agreed to contribute money for necropsy. Part of the money goes to the physician doing the work and part of it goes to the family to aid in burial expenses." - Dr. Wenger, director of the PHS Venereal Disease Clinic in Hot Springs, Arkansas,
in the Hot Springs Seminar (1950) |
"In 1958, along with $25.00 for each year had been in the study, this certificate was sent by name to the remaining study "subjects" by the Public Health Service, signed by Dr. Leroy E. Burney, the U.S surgeon general." (National Archives n.d.)
|
PENICILLIN
"Withholding penicillin marked a medical and moral rupture with the Study's subjects."
- Barbara Rosenkrantz, author of "Non Random Events" (1983)
|
Though penicillin was introduced as a competent treatment for syphilis in the 1940s, the USPHS continued to deny medication to study participants.
"In 1943 Dr. Heller became the director of the Division of Venereal Diseases and could have given penicillin to the subjects and stopped the study. Dr. Heller and subsequent directors of the venereal disease division bear moral responsibility for deliberately shortening the lifespans and inflicting remediable human suffering"
- John C. Fletcher, former director of the Center for Biomedical Ethics at the University of Virginia, in "A Case Study in Historical Relativism" (2000)
|
In 1946, 14 years of non-treatment had elapsed. Penicillin, hailed as the miracle drug, was then available and utilized for the treatment of syphilis ... It was calculated by actuaries that at age 25 black male syphilitics allowed to remain untreated would have reduction in life expectancy of approximately 20%." - Vernal G. Cave, physician and member of Tuskegee Ad-Hoc Committee (1973)
|
Excerpt from a lecture by Frank Snowden, Professor of History at Yale
|
Charles Pollard, a patient in the study, was directly denied syphilitic treatment at hospitals:
"I was fixing to say I was booked to go to Birmingham when this penicillin come out, but the nurse told me I wasn't able to go up there. So they turned me down. I [said] don't want no more part of it."
- Charles Pollard, participant in the Tuskegee Syphilis Study (1973)
Meanwhile, the USPHS collaborated with local physicians to restrict surviving patients from treatment, as it would "contaminate" the study data. To maintain patient cooperation, the USPHS gave participants supplies of ineffective medicines, such as aspirin and vitamins.
THE NUREMBERG CODE
Despite the establishment of the 1947 Nuremberg Code, which set a foundation for international bioethics principles, the USPHS study continued to deny the right of informed consent to its patients.
"The voluntary consent of the human subject is absolutely essential ... The duty and responsibility for ascertaining the quality of the consent rests upon each individual who initiates, directs or engages in the experiment. It is a personal duty and responsibility which may not be delegated to another with impunity ... During the course of the experiment the human subject should be at liberty to bring the experiment to an end if he has reached the physical or mental state where continuation of the experiment seems to him to be impossible."
- Nuremberg Code (1947)